When your doctor confirms that you have uterine fibroids, your first instinct is likely to ask what it is going to take to get rid of them. This is especially true if you are already experiencing symptoms such as heavy and prolonged menstrual bleeding, cramping, pelvic pain, and bloating. These and other fibroid symptoms will only get worse the longer they go untreated, so why not tackle it now? The answer to that question is, you are right! And the good news is that your doctor can present you with multiple treatment options. That said, a combination of relief, worry, and a flood of questions tends to follow—about pain, recovery time, fertility, and yes, what your body will look like afterward. For many women, fibroid surgery scars become part of that conversation sooner than expected.
This is not to suggest that surgery will automatically be the best or only option for every woman. That said, when a procedure is recommended or chosen, it is important to have realistic expectations about healing and scarring. Fibroid surgery scars can vary widely depending on the approach, ranging from procedures like hysterectomy or myomectomy that require abdominal or laparoscopic incisions to minimally invasive treatments like uterine fibroid embolization (UFE) that leave little to no visible marks.
One of our goals at Fibroid Institute is to help as many women as possible understand each treatment option and how those procedures may affect their bodies during recovery. In doing so, they can make a more informed and confident decision. So, let us take a closer look at how myomectomy, hysterectomy, and uterine fibroid embolization differ when it comes to fibroid surgery scars, recovery time, and what most women can realistically expect.
Hysterectomy: What Fibroid Surgery Scars to Expect
Hysterectomies are a common and permanent fibroid removal procedure, so much so that by age 60, one in every three women with symptomatic fibroids will have had one of these surgeries. To put that statistic into a better context, a hysterectomy is currently the second most common gynecological surgery after a C-section. By removing all or part of a woman’s uterus and, in some cases the fallopian tubes and ovaries, fibroids no longer have a viable place to multiply, grow, and cause discomfort.
That said, this is a major surgical procedure that traditionally involves extensive tissue and muscle cutting and will require time to regain strength and function. It can also require hormone replacement therapy (HRT) to manage symptoms and reduce long-term health risks. During recovery, you will likely be under strict bed rest for the first few weeks and should not lift anything heavy throughout recovery.
A hysterectomy can be performed through the vagina, abdomen, or laparoscopically. Furthermore, there are generally three approaches depending on the patient’s unique needs:
- Partial hysterectomy — Your doctor will only remove part of the uterus and possibly ovaries while keeping the cervix intact. You will no longer be able to have children, though it is possible that your ovaries could keep producing hormones until menopause.
- Total hysterectomy — With this procedure, the entire uterus and cervix are removed. Fallopian tubes and ovaries will likely also be removed in cases where a cancer threat is highest.
- Radical hysterectomy — This procedure is reserved for extreme cases where cervical or uterine cancer is present. It involves removing the uterus, the cervix and its surrounding tissue, and the upper part of the vagina. The fallopian tubes and the ovaries may or may not be removed.
Once the type of hysterectomy is determined, the procedure itself follows a predictable sequence. You will be placed under general anesthesia, meaning you will be fully asleep. What happens next—and what your fibroid surgery scars will ultimately look like—depends entirely on the surgical approach used.
Abdominal hysterectomy
- Your surgeon will make a single, large incision (typically 5-7 inches long).
- The incision can be made either horizontally along the bikini line or vertically.
- The uterus and possibly the fallopian tubes are removed.
- The incision is closed with sutures or staples.
- You will be left with a large, permanent scar that may fade but remains visible.
- Recovery time can take six weeks or longer, including a short hospital stay.
Laparoscopic hysterectomy
- Your surgeon will make three to four smaller incisions (roughly 5-10 millimeters).
- The incisions are usually near the belly button and lower abdomen.
- Miniature cameras and surgical instruments help guide the surgeon as the uterus is removed in sections.
- The incision is closed with sutures or staples.
- You will be left with several small scars that can fade over time.
- Recovery time is shorter, at two to four weeks, including a short hospital stay.
Vaginal hysterectomy
- No incisions are made. You will not have any fibroid surgery scars.
- Your surgeon removes the uterus through the vaginal canal.
- Patients experience less pain and reduced recovery time, usually two to four weeks.
- It should be noted that this procedure option is not appropriate for every woman, particularly those who have several large fibroids in different locations in and around the uterus.
Myomectomy: What Fibroid Surgery Scars to Expect
A myomectomy is like a hysterectomy, except that the goal is to remove the symptom-causing fibroids and preserve the uterus. Approximately 30,000 of these invasive surgical procedures are performed annually. Depending on how many fibroids need to be removed, your doctor will surgically reconstruct the uterus to ensure its viability long term. This is good news to women who are not quite ready to have their entire uterus and, in some cases, fallopian tubes and ovaries, removed by way of a hysterectomy, as doing so eliminates their ability to have children in the future.
That said, this is still very much a complex surgical procedure that requires large incisions and a traditionally lengthy recovery time. The typical recovery time is two to six weeks, as myomectomy removes only the fibroids rather than the host structures and is significantly less complex.
There are three ways to perform a myomectomy:
- Hysteroscopic myomectomy — Your doctor relies on a thin, telescopic tube to access the uterine cavity before lifting the walls of the uterus to shave off the fibroids. The recovery time is between one and two weeks.
- Laparoscopic myomectomy — This form of myomectomy only requires four small incisions in the abdominal area, and recovery time is roughly four weeks with minimal scarring.
- Abdominal myomectomy — These are the most common form of myomectomies and require long incisions in the lower abdominal region and in the area of the uterus where the fibroids are located. In these situations, many of the fibroids they are targeting are deeply embedded, which increases recovery time for fibroid treatment.
Once a myomectomy is recommended, the surgical workflow is similar regardless of approach. You will be placed under general anesthesia. Because the uterus remains intact, extra attention is given to closing incision sites within the uterine muscle, which affects both recovery time and the formation of fibroid surgery scars.

Hysteroscopic Myomectomy
- No incisions are made. You will not have any fibroid surgery scars.
- A telescopic tube is inserted through the vagina to guide the surgeon as the fibroids are removed one by one.
- Recovery time is roughly one to two weeks.
Laparoscopic Myomectomy
- Your surgeon will make three to four small incisions (approximately 1/4 to 1/2 inch long).
- The incisions are usually near the lower abdomen.
- Miniature cameras and surgical instruments help guide the surgeon as the uterus is removed in sections.
- The incision is closed with sutures or staples.
- You will be left with several small scars that can fade over time.
- Recovery time is roughly four weeks, and many women return home the same day or after one night.
Abdominal Myomectomy
- Your surgeon will make a single, large incision (typically 5-7 inches long).
- The incision can be made either horizontally along the bikini line or vertically.
- The uterus and possibly the fallopian tubes are removed.
- The incision is closed with sutures or staples.
- You will be left with a large, permanent scar that may fade but remains visible.
- Recovery time can take four to six weeks, including a short hospital stay.
Uterine Fibroid Embolization: What Fibroid Surgery Scars to Expect
Uterine fibroid embolization has become the gold standard for fibroid treatment. Why? It is not fibroid surgery. Rather than physically removing fibroids through invasive and bloody surgical incisions, UFE blocks blood flow to the fibroids. Without this blood supply, fibroids no longer have what they need to thrive inside your uterus. As a result, they naturally shrink and die—thus eliminating painful symptoms.

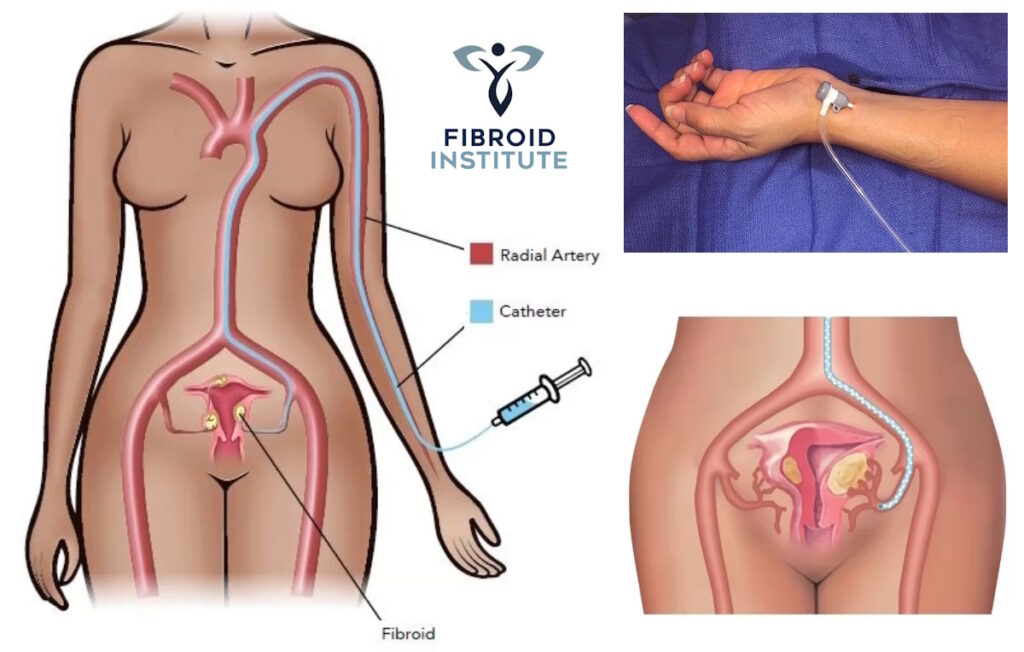
There are two methods for performing UFE: through the wrist or the femoral artery in the groin.
Femoral UFE
- Your doctor makes a small puncture (about 1/4 inch or less).
- The doctor then inserts a catheter into the femoral artery in the groin.
- The catheter is guided to the blood vessels that feed uterine fibroids.
- Only the blood supply to the fibroids is blocked. As a result, the fibroids shrink and die.
- There is no removal of fibroids from your body.
- Since the puncture area is so small, stitches are generally not required.
- There is no hospital stay or fibroid surgery scars.
Radial UFE
As UFE has been fine-tuned over the years, the radial artery is strong viable option. Granted, using the radial approach requires doctors to guide the catheter along a longer path, as this artery runs along the inside of the forearm from the elbow to the thumb. As a result, the catheter must travel up the arm and through the body to the uterine artery. That said, modern medical technology and X-ray-guided imagery have advanced tremendously over the years. Catheters have also become smaller, enabling quick, painless access. On top of that, finding an interventional radiologist who is highly experienced and an expert with this technique, plus has managed thousands of cases through the years, is someone you will want in your corner.
- Your interventional radiologist makes an even smaller puncture on the wrist.
- Tiny particles are injected into the body by a catheter.
- The embolic material blocks nonessential blood vessels leading to the fibroids, which then shrink and die.
- There is no removal of fibroids from your body.
- Since the puncture area is so small, just a dot on the wrist, stitches are generally not required.
- There is no hospital stay or fibroid surgery scars.
A study published in the American Journal of Obstetrics & Gynecology compared 149 UFE patients with 60 myomectomy patients and found similar improvements in symptoms following treatment. In fact, nearly 90% of women report being satisfied with the UFE procedure or remaining free of fibroid symptoms two years after treatment, and a similar percentage report they are still happy with their results five years after treatment.
Fibroid Institute Is Your Answer for Fibroid Treatment Without Surgery
It used to be that fibroid surgery was the only option for women seeking relief from their uterine fibroids. And in some cases, it may still be the best option for certain women. That said, today women are more educated than ever about their fibroid treatment options and what to expect about their recovery, fibroid surgery scars, and more. They are seeking second opinions to ensure they have the correct information and can make informed decisions for their own healing journey.
With the advancement of modern medical technology, minimally invasive procedures such as uterine fibroid embolization have been thrust into the spotlight. The good news is that UFE is non-surgical, offers faster recovery, and delivers effective results. The only decision remaining is to select the right interventional radiologist for UFE care. Beyond the procedure itself, women want a doctor who provides access, communication, comfort, innovation, trust, and a supportive experience from start to finish. Fibroid Institute is here to offer you just that.
In addition, we simplify your UFE journey, managing everything from insurance to PCP communication and offering all patients physician-direct access before and after their procedure. Our fibroid doctors are board-certified interventional radiologists and experts passionate about helping women become #FibroidFree. The bottom line is that you do not have to worry about missing work and life events with every fibroid treatment procedure.
Becoming Symptom Free Is As Easy as one, two, three …

Whether UFE is the right option for you or not, our team of fibroid doctors is always on hand to partner with you and your primary care physician to determine the best course of action. At Fibroid Institute, we do not believe you need to decide between suffering in silence and having invasive surgery.
Request a free 10-15-minute phone screening to determine if you are eligible. If you qualify for UFE after the screening, you can schedule your on-site or telehealth consultation. Most major medical insurance providers cover the cost of UFE. Get started now with the Fibroid Institute in Dallas, Texas at 214-838-6440, in Houston, Texas at 713-903-3733, in South Carolina at 843-628-4290 or complete the form below.
"*" indicates required fields
The Fibroid Institute serves the Charleston, South Carolina, Dallas/Fort Worth, Texas and Greater Houston, Texas metro areas including Addison, Allen, Arlington, Bedford, Bellaire, Carrollton, Cedar Hill, Charleston, Clear Lake, Cockrell Hill, Conroe, Craig Ranch, Cypress, Dallas, DeSoto, Duncanville, Euless, Fort Worth, Frisco, Garland, Grand Prairie, Highland Park, Houston, Hurst, Hutchins, Irving, Katy, Kingwood, Lancaster, League City, McKinney, Mesquite, Mt. Pleasant, Murrells Inlet, Orangeburg, Park Cities, Plano, Richardson, Sherman, Spring, Stafford, Sugar Land, Summerville, Texas City, The Woodlands, Universal City, University Park, Walterboro, Webster and more.
*Patient names and/or photos may be changed to protect patient confidentiality.
Before starting any new treatment or if you have questions regarding a medical condition, always seek the advice of your doctor or other qualified health provider. This information is not a substitute for professional medical advice.

